


Received: 03-Feb-2022, Manuscript No. IJMAR-22-59705; Editor assigned: 05-Feb-2022, Pre QC No. IJMAR-22-59705 (PQ); Reviewed: 17-Feb-2022, QC No. IJMAR-22-59705; Revised: 22-Feb-2022, Manuscript No. IJMAR-22-59705 (R); Published: 01-Mar-2022, DOI: 10.15651/ IJMAR.22.1.4
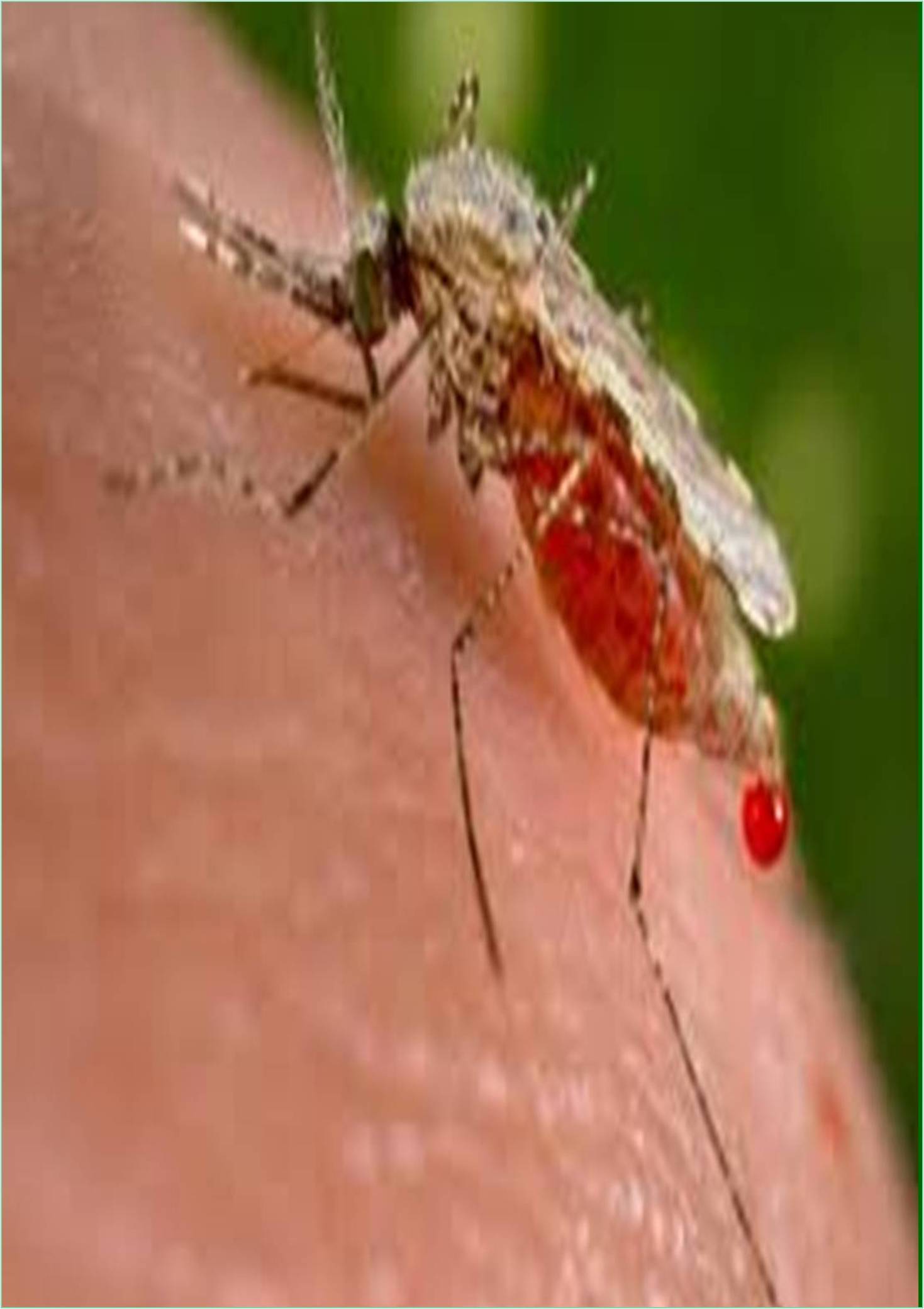
In endemic countries, accurate and timely diagnosis of malaria plays an important role in timely treatment and overcoming the risk of fatal consequences. Peripheral blood smear is a simple technique that can reveal the presence of Plasmodium within hours of blood collection and, in most cases, allows identification of the species involved. Estimates of parasite density are also provided. Also, if no parasites are detected on the first blood smear, a total of 3 sets should be repeated every 12-24 hours. If all 23 sets are negative, this diagnosis can be ruled out. The life cycle of the malarial parasite includes two hosts: insects (e.g. female Anopheles) and vertebrates (e.g. human).
In humans, when a female insect (which develops the reproductive cycle) ingests blood meal, the infected individual ingests gamete mother cells. When an infected female insect injects sporozoite into the host during blood meal, it infects humans (where the asexual cycle occurs).
Types of Smear Blood Malaria
There are several ways to diagnose malaria, but one of the quickest is to look at the patient's blood smear under a microscope. This allows you to identify the presence and type of malaria. Using 50 or more parasitic red blood cells / μL blood samples, malaria can be diagnosed with approximately 70% sensitivity. In how can blood smear be used to distinguish between different types of malaria? Now, each type of malaria has its own characteristics that can be seen under a microscope. Let's take a closer look at how to identify each of the four major types of malaria: Plasmodium falciparum, Plasmodium malaria, Oval malaria, and Malaria parasite.
Malaria is a treatable illness, but lack of rapid and accurate diagnosis and treatment can lead to serious health complications, including death. Microscopic visual inspection of stained thick and thin blood sections is the gold standard for malaria diagnosis. However, the accuracy of microscope-based diagnostics depends largely on the reading experience and attention of individual slides during the diagnostic procedure. In addition, the lack of well-trained staff leads to inconsistencies in the effectiveness of microscope-based diagnostics in malaria-endemic and resource-depleted areas, especially in rural Africa. Inaccurate diagnosis results lead to morbidity, socio-economic problems in society, and inadequate decision-making and planning in malaria prophylaxis programs.
Sporozoite Method
The procedure was reviewed by the local ethics committee, and was in line with the Declaration of Helsinki. Blood samples were taken twice daily from day 6 to day 14 and then daily until day 21. At least 100 highpower fields of thick film were displayed and quantitative PCR was performed on each sample. Volunteers were treated when a single parasite was found on the blood membrane after the presence of the parasite was confirmed by a second microscopist. Neither the attending physician nor the microscopist was aware of the PCR data being studied.
Thick Blood Smear
Giemsa stain was used in the first two sporozoite challenge studies, and field staining of quartz glass was used in the latter two studies. The thick film was air dried by both methods. For Giemsa stain, the film was stored in 5% giemsa for 30 minutes, and then gently washed with tap water and air dried. Soak the slides in field stain A for 3 seconds, then in tap water for 3 seconds (with gentle shaking), soak in field stain B for another 3 seconds, and gently wash with tap water to remove excess stain. The slides were then air dried for at least 30 minutes. The chief microscopist examined the slides prepared by serial dilution without knowing the source. The average thick film uses 10 μL of blood that spreads over 1,000 highpower fields, so 100 high-power fields that are routinely examined during observation make up 1 μL of blood.